What is Ringworm (Tinea)? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Ringworm is not actually a worm — it is a fungal infection caused by microscopic fungi called dermatophytes. Despite the misleading name, the condition is incredibly common and can affect the skin, hair and nails anywhere on the body.
In this article, we explain exactly what tinea infections are, the different types, what causes them, and what you can do about them.
What is ringworm (tinea)?
Tinea is the medical umbrella term for fungal infections caused by dermatophytes — fungi that feed on keratin, the protein found in skin, hair and nails. These fungi thrive in warm, moist environments and can spread from person to person, from animals to humans, or from contaminated surfaces.
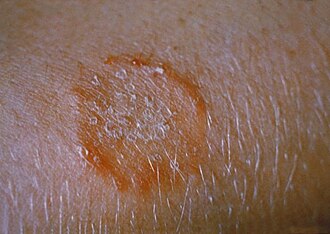
The term "ringworm" comes from the classic ring-shaped appearance of the infection on the body — not from any parasitic worm. It is in fact a fungal infection treated with antifungal medications.
The medical classification is ICD-11: 1F28 Dermatophytosis.
The different types of tinea infections
Tinea is named according to the body part affected:
- Tinea corporis (ringworm of the body): The classic circular, red, itchy patch on the skin with a raised edge and often a clear centre. The most recognisable type.
- Tinea cruris (jock itch): Affects the groin area and inner thighs. Causes intense itching, burning and redness — most frequent in men and people who sweat heavily.
- Tinea pedis (athlete's foot): Typically develops between the toes and on the sole of the foot. Causes itching, burning, scaling and sometimes blistering. The most widespread type of tinea globally.
- Tinea capitis (ringworm of the scalp): Primarily a childhood problem. Causes scaly, itchy patches on the scalp, hair loss and broken hair shafts. Requires oral antifungal medication — creams are not sufficient.
- Tinea unguium / onychomycosis (nail infection): Affects toenails and fingernails, which become discoloured (yellow/brown), thickened, brittle and crumbly. The most difficult type to treat — requires prolonged treatment.
What does ringworm look like?
The appearance depends on the type, but general characteristics include:
- Circular, red, itchy patches with raised borders — classic for tinea corporis
- Scaling and flaking skin — particularly with athlete's foot
- Blisters or small bumps can develop in certain cases
- Hair loss and broken hairs with scalp infection
- Discoloured, thickened and crumbly nails with nail infection
Important: the central area of a ringworm patch often clears up over time while the edge continues to spread — this creates the characteristic ring effect.
Why do tinea infections happen?
Warm and moist environments
Dermatophytes thrive optimally in warm, moist environments. Heavy sweating, tight-fitting clothing and activities involving prolonged moisture (e.g. swimming, intensive sport) significantly increase the risk. Locker rooms, shared showers and swimming pools are classic transmission sites.
Transmission from animals
Cats, dogs, cattle and rodents can all carry dermatophytes and transmit them to humans through direct contact. Infected animals do not necessarily show visible symptoms — an apparently healthy cat can still transmit ringworm.
Sharing personal items
Towels, sports equipment, combs and brushes, shoes and socks can all transfer the fungus. This is a common route of transmission, particularly in families with school-aged children.
Weakened immune system
People with a weakened immune system — e.g. due to HIV/AIDS, diabetes, chemotherapy or immunosuppressive medication — are more vulnerable to tinea infections and may experience more widespread or severe outbreaks.
Who gets tinea infections?
Tinea can affect anyone, but certain groups are more susceptible:
- Children: Particularly prone to tinea capitis (scalp ringworm) due to close contact in schools and nurseries.
- Athletes and active people: The combination of sweat, close contact and shared facilities significantly increases the risk of athlete's foot and jock itch.
- People in close-quarters settings: Dormitories, military barracks and nursing homes are high-risk environments due to shared sanitary facilities.
- Immunocompromised individuals: Illness or medications that weaken the immune system increase both the risk and severity.
- Pet owners: Close contact with cats and dogs that carry dermatophytes.
What can you do about ringworm?
The good news: tinea infections are almost always treatable. The choice of treatment depends on the type and severity:
🧴 Topical antifungals (mild to moderate infection)
Creams and ointments containing clotrimazole, miconazole, terbinafine or ketoconazole are effective for tinea corporis, tinea cruris and mild athlete's foot. Treatment should continue for at least 2 weeks after symptoms disappear.
💊 Oral antifungal treatment (severe or stubborn infection)
Tinea capitis always requires oral treatment (typically griseofulvin or terbinafine). Nail infection (onychomycosis) is treated with oral terbinafine or itraconazole over 3–6 months. Prescription required.
🧼 Hygiene and prevention
Wash and dry affected areas thoroughly. Avoid sharing towels, shoes and clothing. Wear sandals in locker rooms and at public bathing facilities. Change socks and underwear daily and choose breathable fabrics.
🐾 Treat infected pets
If your cat or dog is the source of infection, the animal must be treated by a veterinarian, otherwise reinfections will continue.
Medical classification: Tinea infections are classified as 1F28 Dermatophytosis in the WHO's International Classification of Diseases (ICD-11). They are characterised by annular, scaly plaques caused by dermatophyte fungi and are primarily treated with topical or oral antifungals.
Frequently asked questions
Is ringworm contagious?
Yes. Ringworm spreads easily through direct skin contact with an infected person, via infected animals, or through contaminated objects such as towels, shoes and floor surfaces. Good hand hygiene and avoiding sharing personal items reduces the risk of transmission.
Can ringworm go away on its own?
Very rarely. Most tinea infections require active treatment with antifungal medications. Without treatment the infection will typically worsen and can be transferred to others. Nail infection and scalp ringworm always require prescription treatment.
When should I contact a dermatologist?
Contact a dermatologist if the infection does not improve after 2-3 weeks of over-the-counter treatment, if the infection is widespread or affects the scalp or nails, if you are immunocompromised, or if you are uncertain about the diagnosis. SKIND gives you access to a certified dermatologist within 48 hours.
Get a diagnosis within 48 hours
Upload photos of your skin via the SKIND app and receive a personal diagnosis and treatment plan from a certified dermatologist — no hospital waiting list.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a dermatologist for personal guidance.