What is Psoriasis? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Psoriasis is a chronic, autoimmune skin disease that affects millions of people worldwide. The condition causes skin cells to multiply at an unusually fast rate, resulting in red, scaly patches that are often itchy and can be painful.
In this article, we explain exactly what psoriasis is, how it differs from other skin conditions, what causes it, and what treatment options are available.
What is psoriasis?
Psoriasis is a chronic, autoimmune disease that primarily affects the skin. In psoriasis, the immune system mistakenly attacks healthy skin cells, causing them to multiply at a rate up to 10 times faster than normal. The excess skin cells build up on the surface, forming the characteristic red, scaly patches.
Psoriasis is a systemic disease, meaning it affects the entire body — not just the skin. Up to 30% of people with psoriasis also develop psoriatic arthritis, an inflammatory joint disease that can affect joints and tendons.
Types of psoriasis
There are several different types of psoriasis, each with their own characteristics:
- Plaque psoriasis: The most common form, appearing as raised, red patches covered with silvery scales. Up to 80% of psoriasis patients have this type.
- Guttate psoriasis: Drop-shaped, small red spots, often triggered by streptococcal infections. Most common in children and young adults.
- Inverse psoriasis: Smooth, red skin in body folds such as armpits, groin and under the breasts.
- Pustular psoriasis: White blisters filled with pus surrounded by red skin. Can be localized or generalized.
- Erythrodermic psoriasis: A rare, severe form that covers the entire body with redness and scaling. Requires immediate medical attention.
Symptoms of psoriasis
Psoriasis symptoms vary from person to person, but the most common signs include:
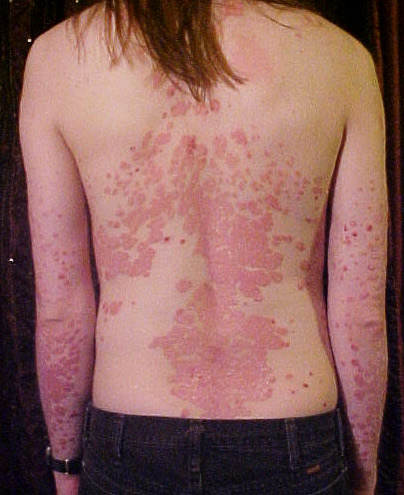
- Red, raised skin patches covered with silvery scales
- Small, drop-shaped spots (guttate psoriasis)
- Dry, cracked skin that may bleed
- Itching, burning or soreness
- Thickened or ridged nails
- Swollen and stiff joints (psoriatic arthritis)
What causes psoriasis?
The exact cause of psoriasis is not fully understood, but research points to a combination of genetic factors and immune system response:
The immune system
Psoriasis is primarily an autoimmune disease. The immune system's T-cells (white blood cells) mistakenly attack healthy skin cells as if defending the body against infection. This triggers a cascade of immune reactions that cause skin cells to multiply faster than normal.
Genetics
Heredity plays an important role. Up to 40% of people with psoriasis have at least one family member with the same condition. Scientists have identified several genes associated with psoriasis, including HLA-Cw6.
Trigger factors
Many factors can trigger or worsen psoriasis:
- Stress: Psychological stress is one of the most common triggers.
- Skin injuries: Cuts, scrapes, sunburns and vaccinations can trigger psoriasis (Koebner phenomenon).
- Infections: Strep throat and other infections can trigger especially guttate psoriasis.
- Medications: Lithium, blood pressure medications (beta-blockers) and antimalarial drugs can worsen psoriasis.
- Weather: Cold, dry weather can worsen symptoms, while sunlight often improves them.
- Alcohol and smoking: Increases the risk of psoriasis and can make treatment less effective.
Treatment of psoriasis
Although psoriasis cannot be cured, effective treatments exist that can control symptoms and improve quality of life:
Topical treatment
For mild to moderate psoriasis, topical treatments are often the first choice:
- Corticosteroids: Reduce inflammation and itching. Available in creams, ointments, gels and lotions of varying strengths.
- Vitamin D analogues: Slow cell growth and scaling, e.g. calcipotriol.
- Retinoids: Vitamin A derivatives that normalize cell growth.
- Salicylic acid: Removes scales and softens thick skin.
Phototherapy
Phototherapy uses ultraviolet light to slow cell growth:
- NB-UVB: Broadband UVB light, often used for moderate psoriasis.
- Smalspektret UVB: More effective than broadband UVB with fewer side effects.
- PUVA: Combination of psoralen (photosensitizing medication) and UVA light.
Systemic and biologic treatment
For moderate to severe psoriasis, systemic medications and biologic therapies may be necessary:
- Biologics: Newer drugs that specifically target parts of the immune system (TNF-alpha, IL-17, IL-23). Extremely effective with fewer systemic side effects.
- DMARDs: Disease-modifying antirheumatic drugs such as methotrexate and cyclosporine.
- Apremilast: Oral medication that inhibits an enzyme involved in inflammation.
Frequently asked questions
Is psoriasis contagious?
No, psoriasis is not contagious. You cannot get psoriasis by touching someone with the condition, and it is not transmitted through blood or other body fluids.
How does psoriasis affect quality of life?
Psoriasis can have a significant psychological impact due to visible skin changes. Many experience stigmatization, low self-esteem, anxiety and depression. Up to 10% have suicidal thoughts. Early and effective treatment is important.
Diet and lifestyle with psoriasis
While no diet can cure psoriasis, some lifestyle changes can help: maintain a healthy weight, avoid smoking and alcohol, manage stress, and eat an anti-inflammatory diet with omega-3 fatty acids.
Get a diagnosis within 48 hours
If you are experiencing persistent skin changes that could be psoriasis, you can get a personal assessment from a certified dermatologist via the SKIND app — no waiting list.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a dermatologist for personal guidance and assessment of skin changes.