What is Shingles (Herpes Zoster)? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Shingles (herpes zoster) is a painful viral infection that affects around one million people in the US alone each year and is similarly prevalent across Europe. It is not a new infection — it is a reactivation of a virus you already carry.
In this article we explain exactly what shingles is, what causes the reactivation, what it looks like, and what you can do to reduce its duration and the risk of complications.
What is shingles?
Shingles is a viral infection caused by the varicella-zoster virus (VZV) — the same virus responsible for chickenpox (varicella). When you recover from chickenpox, the virus does not die out. It retreats into the nervous system and lies dormant in sensory nerve cells (dorsal root ganglia), potentially for decades.
When the immune system weakens — through age, illness, stress or medication — the virus can reactivate, travel along nerve pathways and reach the skin, where it causes the characteristic shingles rash.
Shingles is not contagious in the same way as chickenpox: you cannot "catch shingles" from someone who has it, but if you have never had chickenpox or are unvaccinated, you can contract VZV from the blisters and subsequently develop chickenpox.
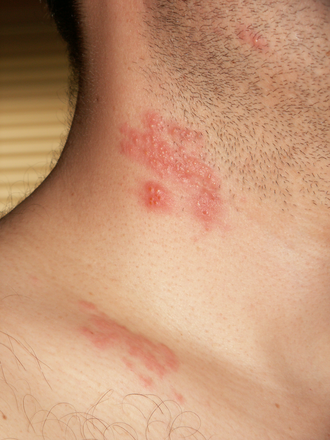
What does shingles look like?
Shingles typically progresses in stages and follows a characteristic pattern:
- Prodromal phase (1–5 days): Burning, tingling or tenderness along a specific part of the body — typically on one side. Fever, fatigue and sensitivity to light may occur.
- Rash phase (2–4 weeks): A painful red rash appears in a band or cluster along the nerve path — most often around the torso, but can affect the face, eyes and mouth. Within a few days fluid-filled blisters develop, which then burst and form yellow crusts.
- Healing phase: The crusts fall off within 2–4 weeks. The skin may leave marks or scars, but this is not always the case.
It is crucial to note that herpes zoster ophthalmicus — shingles near the eye — is a serious condition that can threaten vision and requires immediate medical attention.
Why does shingles happen?
Reactivation of VZV occurs when the immune system is no longer strong enough to keep the virus dormant. The main triggering factors are:
Age
The immune response that keeps VZV dormant naturally weakens with age. The risk of shingles increases markedly after age 50, and more than half of all cases occur in people over 60. Approximately one in three people will develop shingles during their lifetime.
Weakened immune system
Conditions such as HIV/AIDS, autoimmune diseases, cancer and organ transplantation — as well as immunosuppressive therapies — significantly increase the risk of shingles. These individuals may also experience more severe and prolonged outbreaks.
Stress
Severe physical or psychological stress can temporarily weaken the immune system, thereby increasing the risk of VZV reactivation. Many patients can link their first outbreak to a particularly stressful period.
Who gets shingles?
Anyone who has had chickenpox carries VZV and can potentially develop shingles. Certain groups are at particularly high risk:
- Older adults (50+): Risk increases sharply with age. Adults over 80 have 8–10 times the risk compared to those in their 20s.
- Immunocompromised individuals: Cancer patients undergoing treatment, HIV-positive individuals, and those on long-term steroid or biological therapy.
- Those who had chickenpox at a young age: Early chickenpox infection, particularly in the first 12 months of life, is associated with an increased risk of shingles in childhood and young adulthood.
Treatment and prevention
Early treatment is crucial. The sooner you start antiviral therapy, the shorter and milder the outbreak:
💊 Antiviral medications
Aciclovir, valaciclovir or famciclovir should be started within 72 hours of rash onset. They shorten the outbreak and reduce the risk of post-herpetic neuralgia (PHN).
🩺 Pain management
Paracetamol, NSAIDs and in more severe cases opioids, tricyclic antidepressants or gabapentin can be used to manage the often intense pain during and after the outbreak.
💉 Vaccination
The shingles vaccine (recombinant zoster vaccine, Shingrix) is recommended for all adults over 50, even if they have previously had shingles. It reduces the risk of shingles by up to 90% and the risk of PHN by over 85%.
⚠️ Post-herpetic neuralgia (PHN)
PHN is the most common complication of shingles: persistent neuropathic pain lasting months or years after the skin has healed. Early antiviral treatment is the most important preventive factor. Seek help immediately if pain persists after healing.
Medical classification: Shingles is classified as 1E91 Zoster in the WHO's International Classification of Diseases (ICD-11). The condition is characterised by a painful rash with a dermatomal distribution, caused by reactivation of the varicella-zoster virus, and is treated with antivirals and pain management.
Frequently asked questions
Can you get shingles more than once?
Yes. Although most people only experience one outbreak, shingles can recur — particularly in immunocompromised individuals. Vaccination reduces the risk of recurrence.
Is shingles contagious to others?
The virus can only spread from open blisters, not through the air. Individuals who have never had chickenpox or are unvaccinated can contract VZV from the blisters and develop chickenpox — not shingles. Avoid contact with pregnant women, newborns and immunocompromised individuals while blisters are active.
When should I contact a doctor?
Immediately upon suspicion of shingles — especially with a rash near the eye, fever, or severe pain. Antiviral treatment works best within 72 hours of rash onset. SKIND gives you access to a dermatologist within 48 hours.
Get a diagnosis within 48 hours
Upload photos of your skin via the SKIND app and receive a personal diagnosis and treatment plan from a certified dermatologist — no hospital waiting list.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a dermatologist for personal guidance.