What is Herpes Simplex Virus (HSV)? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Herpes simplex virus (HSV) is one of the most widespread viral infections in the world — it is estimated that more than two-thirds of the global population under 50 carry HSV-1. Despite its prevalence, there is still considerable confusion and stigma surrounding the diagnosis.
In this article we explain exactly what HSV is, how HSV-1 differs from HSV-2, what an outbreak looks like, and what you can do about it.
What is herpes simplex virus?
Herpes simplex virus (HSV) is a lifelong viral infection that causes outbreaks of small, painful blisters on the skin and mucous membranes. There are two main types:
- HSV-1: Typically responsible for oral herpes, causing cold sores (herpes labialis) around the mouth and lips. HSV-1 is extremely common and is most often transmitted in childhood through kissing or touching.
- HSV-2: Primarily associated with genital herpes, causing outbreaks on the genitals or surrounding areas. HSV-2 is transmitted almost exclusively through sexual contact.
It is important to understand that HSV is not a reflection of poor hygiene or promiscuous behaviour. The virus is highly contagious and can be transmitted by people who do not know they are infected.
What does an HSV outbreak look like?
An outbreak typically follows a predictable pattern. Many people experience warning symptoms before the blisters appear:
Prodromal phase (warning symptoms)
The outbreak typically begins with tingling, burning, itching or numbness in the affected area — often 1–2 days before the blisters appear. Some people also experience local tenderness or swollen lymph nodes.
Blister phase
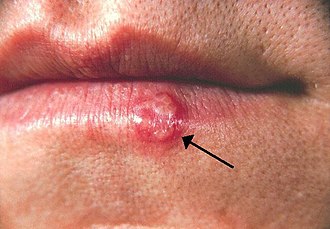
Clusters of small, fluid-filled blisters then appear on a reddened base. The blisters are typically painful. With HSV-1 they usually form at the corner of the mouth or on the lips; with HSV-2 on or around the genitals, buttocks or thighs.
Healing phase
The blisters burst and form ulcers, which are subsequently covered by a crust. Symptoms usually clear within 2–4 weeks during the first outbreak and more quickly during subsequent outbreaks. The skin usually heals without scarring.
Why does it happen — and what triggers outbreaks?
HSV spreads through direct contact with infected skin or bodily fluids. The virus penetrates the skin or mucous membranes and then establishes itself in sensory nerve cells near the spinal cord, where it remains dormant (latent) for life. Certain factors can reactivate the virus and trigger a new outbreak:
- Stress and fatigue: Psychological or physical stress is one of the most common triggers.
- Weakened immune system: Illness, medication (e.g. immunosuppressants) or HIV can increase the frequency of outbreaks.
- Sunlight (UV radiation): Prolonged sun exposure is a well-known trigger for cold sores (HSV-1).
- Hormonal changes: Menstruation can trigger HSV-2 outbreaks in women.
- Febrile illness: Colds, influenza and other infections can reactivate the virus.
Asymptomatic transmission is also possible: the virus can shed from the skin (viral shedding) even without visible blisters, which is why HSV can be transmitted even when there are no visible signs of an outbreak.
Who gets HSV?
HSV is extremely widespread globally:
- HSV-1: The WHO estimates that approximately 67% of the global population under 50 is infected with HSV-1. Most are infected in childhood and never experience symptoms.
- HSV-2: Approximately 11% of the global population under 50 carries HSV-2. Prevalence is higher in women than men.
Many infected individuals never experience noticeable symptoms, or only notice mild signs that they attribute to other causes. HSV can therefore be carried and spread unknowingly.
Treatment and management of HSV
There is currently no cure for HSV — the virus remains in the body for life. However, antiviral medications can shorten outbreaks, reduce symptoms and lower the risk of transmission:
💊 Episodic treatment
Antiviral agents such as aciclovir, valaciclovir or famciclovir are taken at the first signs of an outbreak and significantly shorten the blister phase. The earlier treatment is started, the better the effect.
🛡️ Suppressive therapy (daily antiviral)
For frequent outbreaks (6 or more per year) or to protect a partner, daily antiviral therapy can reduce frequency, duration and transmission risk by up to 50%.
🌞 Trigger prevention
Sunscreen on the lips (SPF 30+), stress management, adequate sleep and general immune support can reduce the number of HSV-1 outbreaks.
🤝 Open communication
It is important to inform sexual partners of the diagnosis and take the necessary precautions (condom use, avoid contact during outbreaks). Open communication is essential for protecting partners and reducing stigma.
Medical classification: Herpes simplex infections are classified as 1F00 in the WHO's International Classification of Diseases (ICD-11). The condition presents as painful vesicles on oral or genital mucosa and is treated primarily with antiviral medications such as aciclovir.
Frequently asked questions
Can you live a normal life with HSV?
Yes. The vast majority of people with HSV live full and active lives. Outbreaks typically become less frequent and milder over time. With appropriate treatment and precautions, transmission risk can be reduced and one can live normally — including in relationships and sexual life.
Are HSV-1 and HSV-2 the same?
They are related but not identical. HSV-1 most often causes oral herpes, while HSV-2 primarily causes genital herpes. HSV-1 can however be transmitted to the genitals through oral sex, and vice versa. Both types are managed with the same antiviral medications.
Do I need to tell my partner about the diagnosis?
Yes, it is important. Open communication about HSV status enables both partners to make informed decisions and take precautions. Remember that the virus can be transmitted even without visible outbreaks (asymptomatic shedding).
When should I contact a dermatologist?
Contact a dermatologist for frequent outbreaks (more than 6 per year), if you are pregnant and have genital herpes, if you are unsure of your diagnosis, or if symptoms are severe. A correct diagnosis and treatment plan is important.
Get a diagnosis within 48 hours
Upload photos of your skin via the SKIND app and receive a personal diagnosis and treatment plan from a certified dermatologist — no hospital waiting list.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a dermatologist for personal guidance.