What is Eczema (Atopic Dermatitis)? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Eczema is one of the most common chronic skin conditions, affecting up to 20% of children and 3% of adults worldwide. The persistent itch and irritation can significantly impact sleep, quality of life and daily well-being.
In this article we explain exactly what eczema is, what causes it, what it looks like, and what you can do about it.
What is eczema?
Atopic dermatitis — commonly known as eczema — is a chronic, inflammatory skin condition that makes the skin red, itchy and sometimes swollen. "Atopic" refers to a hereditary tendency towards allergic reactions, and the condition is closely linked to asthma and hay fever in what is called the atopic triad.
Eczema is not contagious. You cannot spread it to others or catch it from another person. It is an internal condition driven by the immune system and genetics.
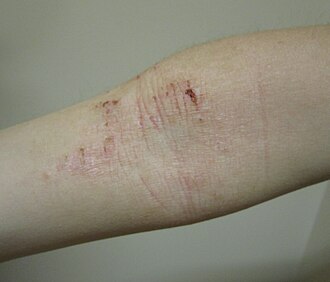
What does eczema look like?
Eczema can look very different depending on a person's age and skin type:
- Dry, scaly patches: Typically on the neck, face and around the eyes in adults. The skin may look rough and dull.
- Redness and swelling: Inflamed areas look red and may feel warm. In darker skin tones, redness may appear as a darker discolouration.
- Intense itching: Itching is often the most troublesome symptom and can worsen at night. Scratching provides temporary relief but worsens the skin and can lead to infection.
- Raw, cracked or bleeding skin: Repeated scratching can lead to open sores and cracks in the skin, increasing the risk of bacterial infections.
- Lichenification: With long-term itching and scratching, the skin can become thicker and leathery — a sign of chronic eczema.
In adults, eczema most commonly affects the elbows, backs of the knees, wrists, neck and face. In infants and young children, it often appears on the face and torso.
Why does eczema happen?
The exact cause of eczema is not fully understood, but research points to a combination of factors:
Impaired skin barrier
In people with eczema, the skin barrier is impaired, making it easier for irritants and allergens to penetrate and for moisture to evaporate out. A mutation in the gene for filaggrin — a protein essential for a healthy skin barrier — is a common cause.
Overactive immune system
The immune system overreacts to seemingly harmless substances such as dust, pet hair or certain foods, triggering an inflammatory response in the skin. This is a similar mechanism to other atopic conditions such as asthma and allergies.
Genetics
Eczema runs in families. If one or both parents have eczema, asthma or hay fever, the risk of the child developing atopic dermatitis is significantly increased.
Triggering factors
Even with a genetic predisposition, eczema often requires a trigger to flare up. Common triggers include:
- Stress and psychological strain
- Weather changes — especially cold, dry weather
- Harsh soaps, fragrances and cleaning products
- Certain foods (e.g. milk, eggs, nuts and gluten-containing products)
- Synthetic fabrics and wool
- Sweat and overheating
Who gets eczema?
Anyone can develop eczema, but it is most common in:
- Infants and children: Up to 20% of all children have atopic dermatitis. The condition often develops in the first year of life and improves for many during childhood or teenage years.
- Adults with family history: Around 3% of adults live with chronic eczema, and many find the condition returns even if it improved in childhood.
- People with an atopic background: If you or your family have allergies, asthma or hay fever, the risk of eczema is higher.
What can you do about eczema?
Eczema cannot be cured, but it can be effectively controlled with the right treatment and skincare routine:
💧 Moisturiser (most important daily treatment)
Apply a rich, fragrance-free moisturiser or emollient at least twice daily — even between flares. This strengthens the skin barrier and reduces the frequency and severity of flares.
🩺 Topical corticosteroids
Corticosteroid creams (cortisone) suppress inflammation and itching during flares. They come in varying strengths — mild to strong — and are prescribed by a dermatologist based on severity and location.
🧪 Immunomodulators (calcineurin inhibitors)
Creams such as tacrolimus and pimecrolimus are a steroid-free alternative for sensitive areas like the face and neck. They suppress the local immune reaction without the side effects that can occur with long-term steroid use.
💊 Systemic treatment (severe eczema)
For severe or widespread eczema, a dermatologist may prescribe biological treatment (e.g. dupilumab), oral immunosuppressants or phototherapy (light therapy).
🚫 Avoid triggers
Identify and avoid your personal triggers. Use fragrance-free products, soft clothing and take short, lukewarm showers rather than long hot baths.
Medical classification: Atopic eczema is classified as EA80 in the WHO's International Classification of Diseases (ICD-11). It is characterised as a chronic, inflammatory condition with itchy, red and dry skin. Treatment includes moisturisers, topical steroids and immunomodulators.
Frequently asked questions
Can eczema disappear completely?
Many children grow out of eczema during their teenage years, but for others it remains a chronic condition requiring ongoing management. With the right treatment, however, eczema can be brought under full control.
Is eczema the same as dry skin?
No. Dry skin can occur in anyone and is caused by a lack of moisture. Eczema, however, is an inflammatory condition with an immunological basis that requires medical treatment beyond simply moisturising.
When should I contact a dermatologist?
Contact a dermatologist if itching is disturbing your sleep, the skin starts to weep or become infected, over-the-counter remedies are not helping, or if eczema is significantly affecting your daily life.
Get a diagnosis within 48 hours
Upload photos of your skin via the SKIND app and receive a personal diagnosis and treatment plan from a certified dermatologist — no hospital waiting list.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a dermatologist for personal guidance.